EnsoData’s Actuarial Analysis of Untreated OSA Reveals the Expansive Impact OSA has on Chronic Comorbid Conditions and Healthcare Costs
The importance of sleep health is no revelation to the field of sleep medicine. Outside of sleep medicine, however, it often goes under the radar. At EnsoData, our hope is to provide sleep professionals with resources to elevate the awareness and importance of sleep health and its effect on healthcare costs and chronic comorbid conditions within health organizations. That’s why we conducted the OSA actuarial study presented in our latest research webinar: The Impact of OSA Therapy on Healthcare Costs. As alluded to in the title, in this EnsoData webinar, EnsoData CEO and Co-Founder, Chris Fernandez, presented insights and takeaways from recent research examining the economic impact of Obstructive Sleep Apnea (OSA) therapy compliance. He covers EnsoData’s motivations behind the research, the collaborators who helped make this research project possible, and the study sample itself, which included over 2 million Medicare patients nationwide. However, the real meat of the presentation comes in the data analysis, including the important relationship between sleep apnea and total medical spend, and more specifically how treated sleep apnea reduces total medical spend by ~20%. To conclude his presentation, Chris outlined the co-prevalence of chronic, high-cost comorbidities and sleep apnea, the impact this research may have, and future work that EnsoData has planned. And you can’t miss the panel-style Q&A session with study collaborators:- Ian Duncan, PhD, FSA, MAAA, Adjunct Professor of Actuarial Statistics, University of California Santa Barbara, President, Santa Barbara Actuaries Inc.
- Nathaniel F. Watson, MD, MSc, Adjunct Professor, Department of Neurological Surgery, University of Washington (UW) School of Medicine, Principal, NeuroSleep LLC
- Jen McClurg, MBA, SVP Payor Solutions, EnsoData
Results from EnsoData’s OSA Actuarial Study
While we’d like to highlight everything from the presentation, the data is comprehensive, and you can only get a little of it without watching the full webinar. Chris covers the healthcare cost averages over the whole Medicare population dataset in comparison to the OSA patient subset. He also looks at three sub-groups of varying degrees of CPAP compliance. After talking through those first two areas of interest, Chris closes by examining the number of concurrent comorbidities associated with OSA. That’s what we’ll share in a little teaser of the presentation. First up, this table provides an overview of the average PMPM, or per-patient-per-month, healthcare costs for the various Medicare populations, broken into quantiles for the full population, 50th percentile of cost, 75th percentile of cost, and 90th highest percentile of cost patients. You can see the stark differences in patients with OSA compared to the overall population in the bottom most row.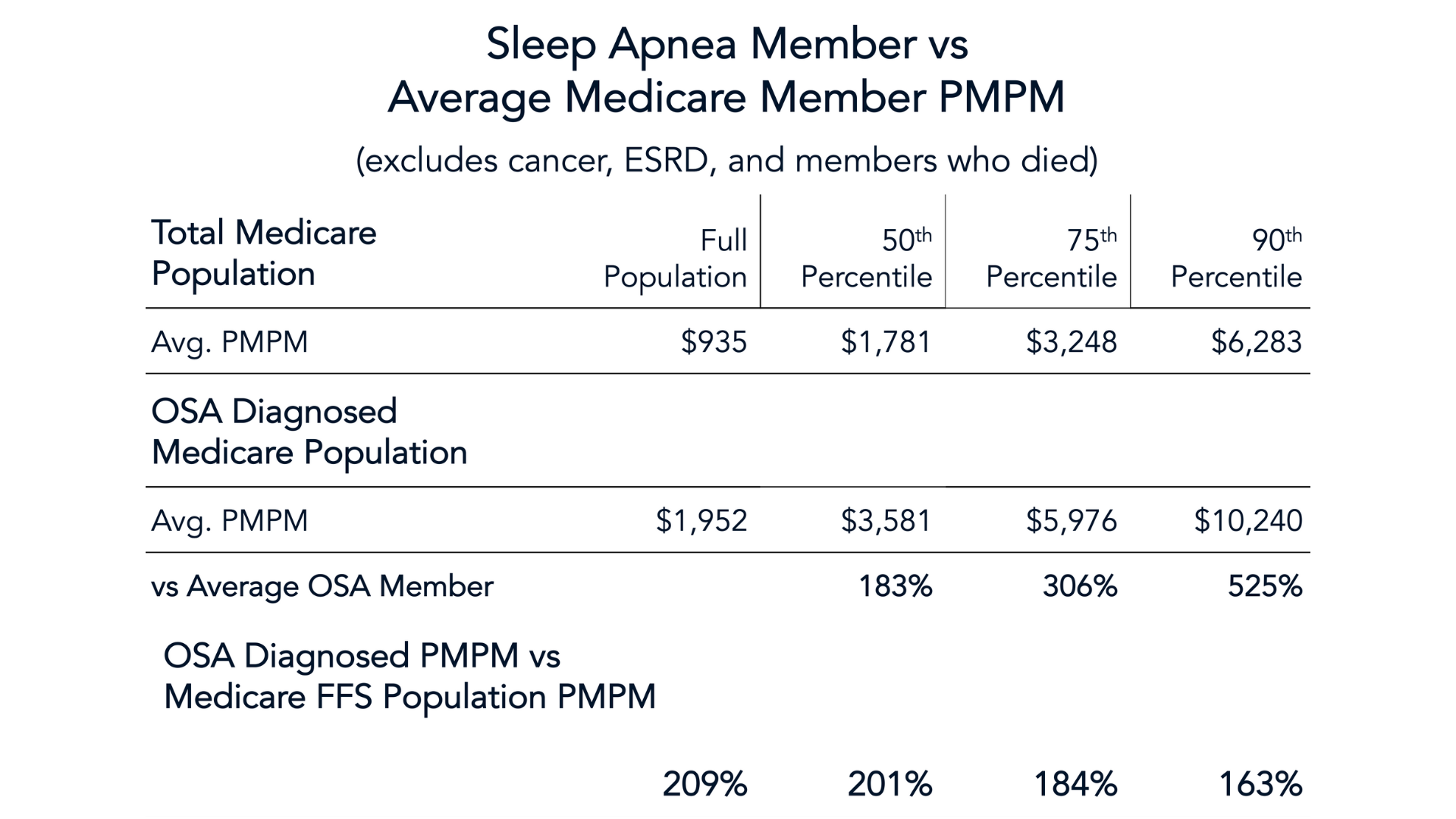 As you can see above, the primary takeaway was that Medicare patients with OSA are 209% more costly.
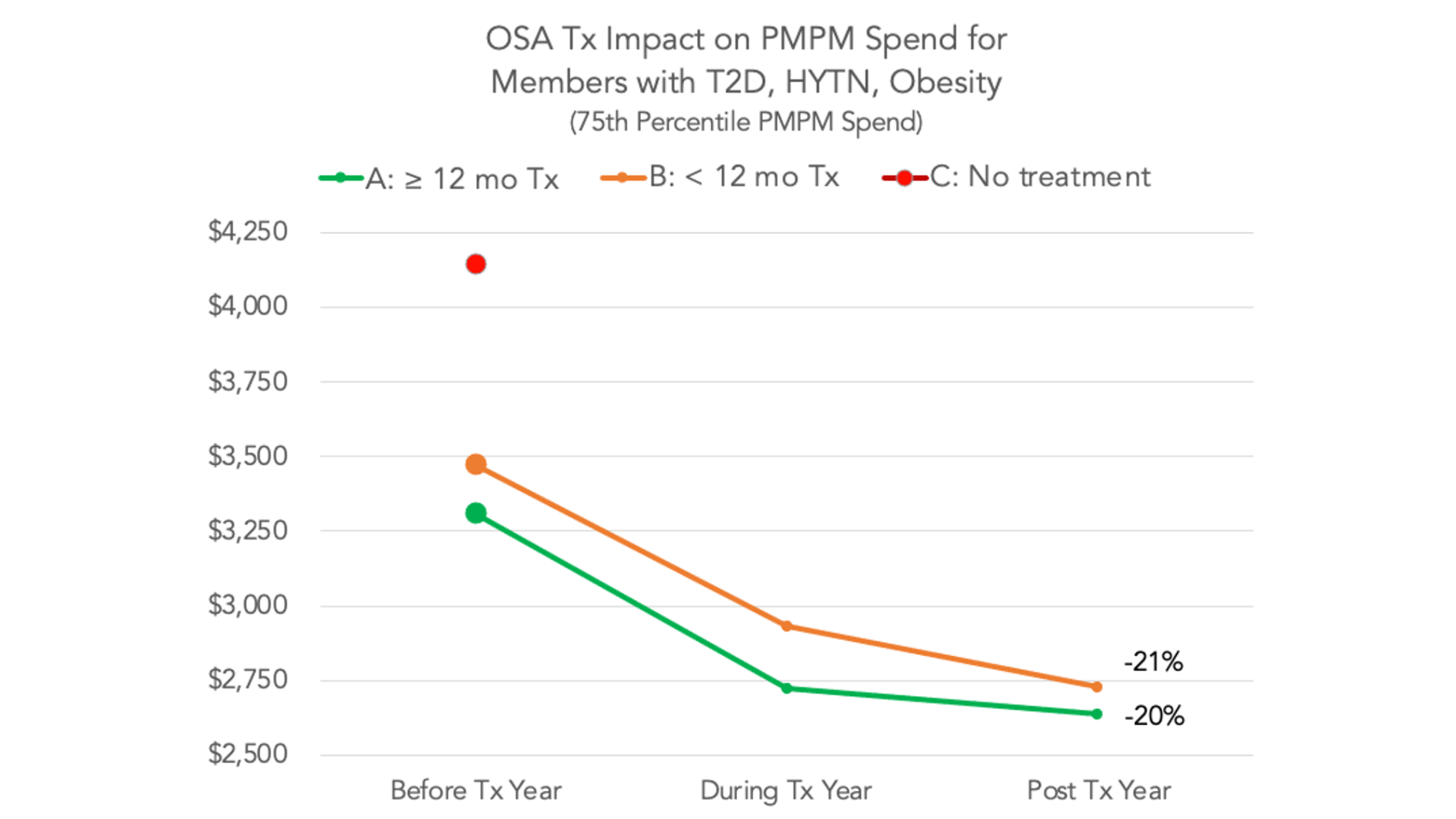
In the next chart below, Chris highlights the decreases in costs for patients after they begin treatment. It’s also clear that patients who maintain adherence to treatment continue to improve when it comes to PMPM costs, as we observed 20% and 21% PMPM reductions between the year before treatment began and in the post treatment year.
As you can see above, the primary takeaway was that Medicare patients with OSA are 209% more costly.
In the next chart below, Chris highlights the decreases in costs for patients after they begin treatment. It’s also clear that patients who maintain adherence to treatment continue to improve when it comes to PMPM costs, as we observed 20% and 21% PMPM reductions between the year before treatment began and in the post treatment year.
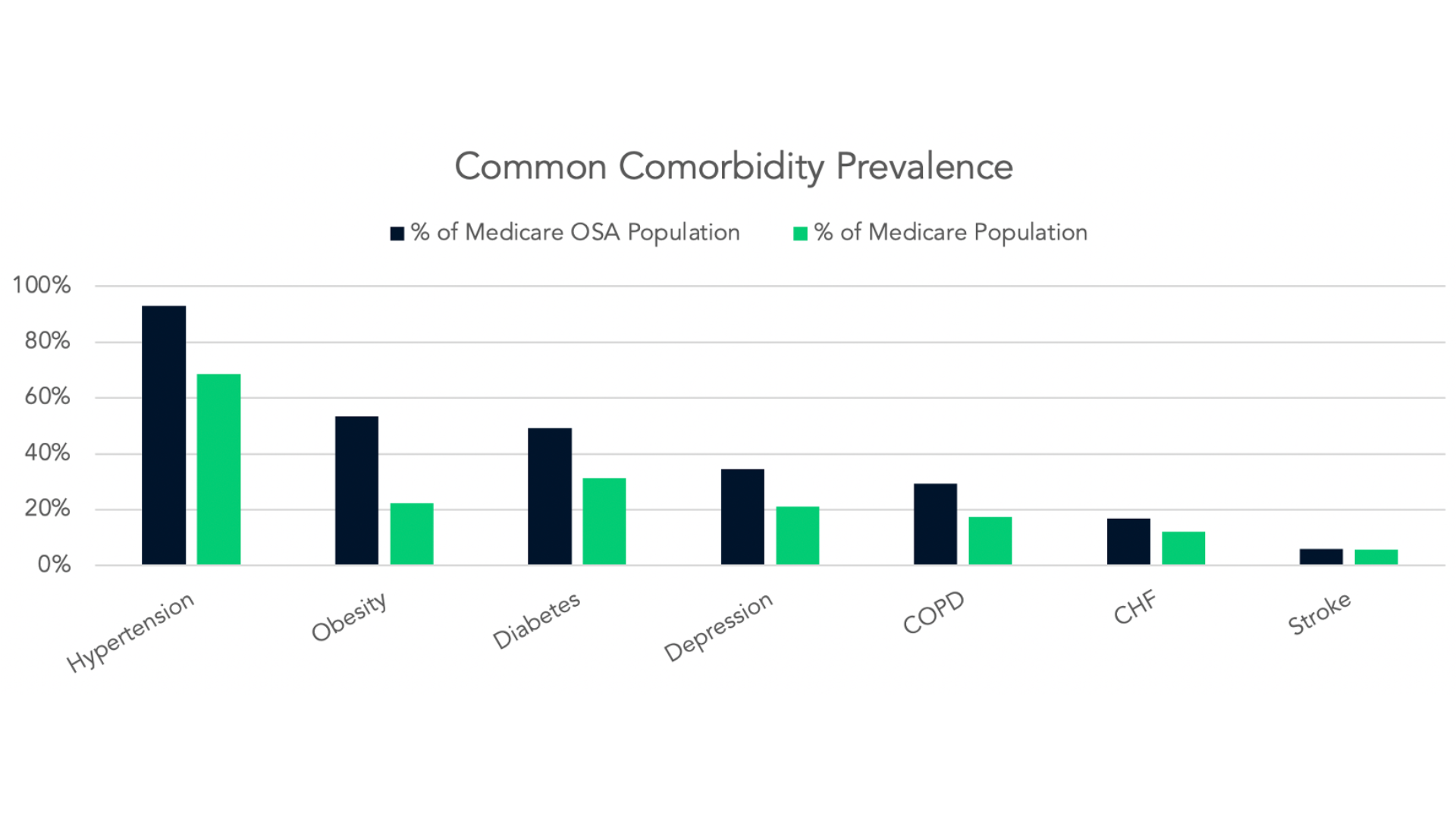
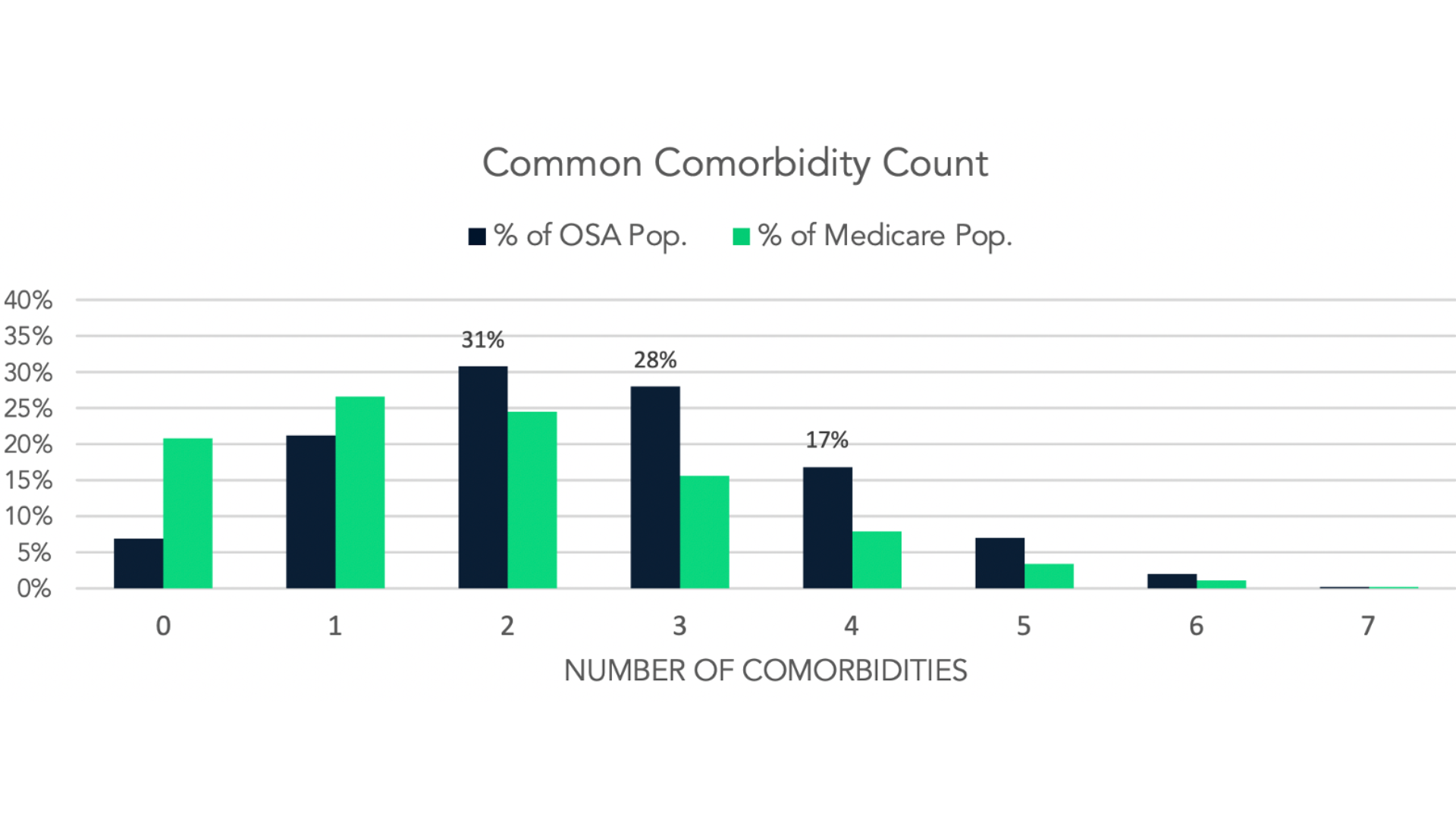
 Next, in the below graph, you can see the common comorbidity count for patients in the data subset. Basically, how many other comorbidities does someone have for each of the disease states, and then more specifically, what those percentages look like when adding in OSA as a comorbidity.
Next, in the below graph, you can see the common comorbidity count for patients in the data subset. Basically, how many other comorbidities does someone have for each of the disease states, and then more specifically, what those percentages look like when adding in OSA as a comorbidity.
 As you can see in the next graph, patients with 2-4 comorbidities account for 76% of the OSA population whereas in the baseline population members with 2-4 comorbidities only account for 48%.
As you can see in the next graph, patients with 2-4 comorbidities account for 76% of the OSA population whereas in the baseline population members with 2-4 comorbidities only account for 48%.
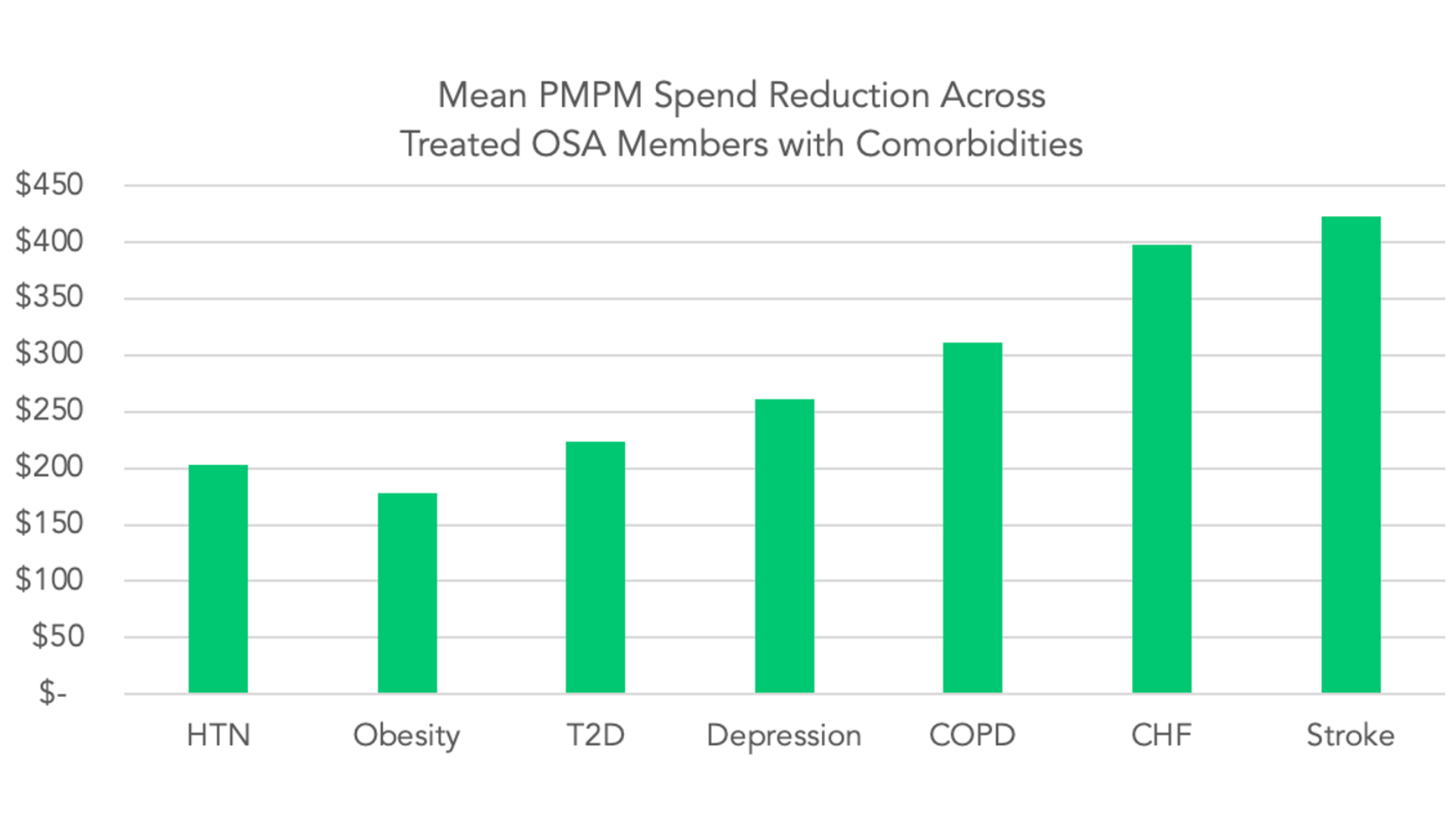 And finally, you can see the value of treating each specific comorbidity. When you remember that 76% of patients with OSA have 2-4 comorbidities, you’re looking at massive savings if you address the OSA which exacerbates these other diseases.
And finally, you can see the value of treating each specific comorbidity. When you remember that 76% of patients with OSA have 2-4 comorbidities, you’re looking at massive savings if you address the OSA which exacerbates these other diseases.
 To listen to the full Q&A section and Chris’ presentation on EnsoData’s OSA Actuarial Study, watch the on-demand webinar now. You can also register for any of our upcoming webinars on our website.
To listen to the full Q&A section and Chris’ presentation on EnsoData’s OSA Actuarial Study, watch the on-demand webinar now. You can also register for any of our upcoming webinars on our website. 





