Meet Susan Smith, the Sleep Clinical Director who Oversees Compliance, DME, and Business Development for Sleep Management Services in Arkansas and Texas
In 2005, our sleep story candidate Susan Smith set out with three associates to create a new sleep experience for patients in Central Arkansas. Flash forward to 2021, and the decision to venture out can be described as nothing but a success, as the Sleep Management Services (SMS) organization flourishes. The southern hospitality that Smith brought to our conversation is the same as she weaved into her organization’s core mission:Our sole focus is providing an excellent patient experience with the goal of treating sleep related problems,” said Smith.
About SMS and Susan Smith
Founded in 2005, SMS employs 50 staff members who support roughly 7,500 patients at more than a dozen locations, primarily in Arkansas, but also in Texas. The team provides a variety of sleep services, including turnkey sleep management for a number of hospital sleep centers. SMS also operates independent AASM accredited diagnostic sleep labs. Because their mission is treating sleep problems, not making sleep diagnoses, the team also prides itself on the treatment services they provide via their provider services and DME divisions. Susan Smith serves as the Sleep Clinical Director, but wears far more hats than just the one. She started in sleep medicine in 1997, as a mom reentering the workforce. At the time, Smith was working as a respiratory therapist, managing the day sleep scoring process, while also performing a lot of the marketing lift, a perk for a working mom when most RT shifts are at night. Beyond serving as the director of clinical sleep services, Smith also leads the DME program and is part of the SMS management team focused on the overall business development process. Like many other sleep stories in this series, Smith had a sleep moment that changed her career trajectory forever. However, unlike some of our other stories (like Laura Linley of Advanced Sleep Management and Tammy Sterner of WellSpan Health), Smith’s moment wasn’t about how she “found” sleep, but rather how she discovered her passion for entrepreneurship and a desire to improve the care continuum for her community.Efficiency, Technology Drive Success at SMS
Everyone on the SMS team works hard to assure patients are cared for and have a good experience. Office staff is friendly and efficient and the technical staff strives to provide the best patient treatment and care. While Smith wouldn’t give away the magic formula for a successful sleep lab, she made it clear that maximizing efficiency is vital. At SMS, the process from receiving the referrals, to sending patients to a DME company, to following up after testing, is streamlined and efficient. How? It’s all in the process, says Smith. Besides efficiency, Smith attributes SMS’s success to technology adoption.Technology has come a long way since I started in sleep 20+ years ago,” said Smith. “I have seen it go from paper analysis to everything electronic. We recently upgraded our EHR which integrates seamlessly with our recording system. Everything we do is electronic, which streamlines processes and helps the environment,” Smith said, adding, “I swear we were killing a forest in 2005. I’d tell my techs, ‘you turn those papers over and use the other side!’ Compare that to today, where we are almost 100% paper-free.”By focusing on improving processes with technology, Smith’s team found themselves on the front line of innovation. That’s what drove SMS to adopt AI scoring.
How AI Scoring Fit into the SMS Equation
When SMS’s CEO, Ryan Smolek, first brought up EnsoData’s AI scoring solution EnsoSleep, Smith was skeptical. As a sleep clinician, one major challenge was overcoming past experiences with other autoscoring solutions. “A clinician at heart, I did not think that there was a scoring software out there that would really assist our scoring team,” said Smith. However, as SMS evaluated EnsoSleep, Smith researched EnsoData and read the published data on AI scoring capabilities. Smith cited the April 2020 JCSM position paper released by the AASM on embracing AI technology for sleep scoring as a turning point. That paper gave her the final push, as Smith decided to follow the advice of the AASM president to “embrace technology” to keep the business of sleep medicine moving forward. Smith’s next hurdle was to convince her scoring staff to accept EnsoSleep and to assure them that technology wasn’t going to replace them.I am happy to say they did embrace the EnsoSleep AI scoring technology, which allowed the scoring team time to focus on quality initiatives with our technical staff,” she said.As outlined by Smith, EnsoSleep provided the scoring staff with more time to devote to other initiatives. This shift in focus has been channeled into a few areas. First, EnsoSleep provides an excellent starting point for the day techs to overscore with time left to focus on training and assisting night staff with any recording quality issues. Electronic paperwork allows more time for set-up at the beginning of an appointment for night staff and because SMS does not score on the fly, techs have more time to monitor the patient’s leads and data quality. Since they have more time to focus on proper lead placement and data collection, the SMS team has begun to set a high standard for data collection among the sleep community.
With Newfound Time, SMS Focuses on Collecting Quality Data
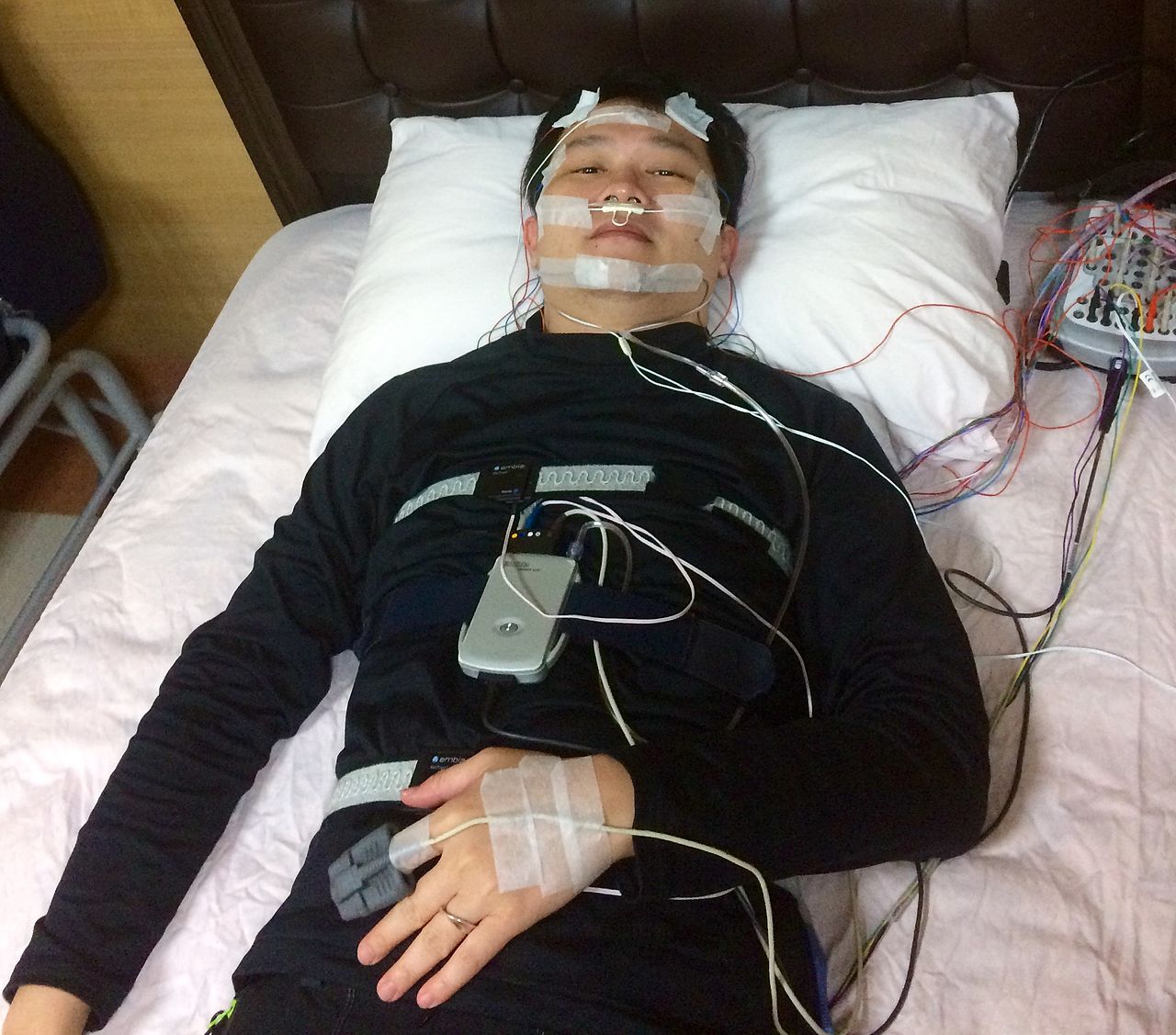 A third area where SMS excels in their use of technology is in the process of gathering sleep data. In a PSG study, the night tech will monitor a patient’s brain waves, eye movements, heart rate, breathing patterns, blood oxygen level, their limb and body movements, as well as any other movements or noises, such as snoring or sleep walking. As part of this process, night techs must monitor a lot of sensors on a person, as demonstrated in the photo to the right.
For the non-sleep techs in our reading audience, among the data points that are gathered in a PSG, a patient will typically have eight EEG leads on their head. In the above photo, you can see two of these eight leads on the forehead, which would translate to F3 and F4 in the below chart. As you can see below, when it comes to collecting data from these specific leads, the SMS team truly stands out, in a good way. Across all eight of the electrodes, their team consistently collects data at a rate higher than their peers.
As you can see below, for the eight signal leads on the head during a PSG, SMS’s signal accuracy is consistently above the 75th percentile among their peers. Not only that, but for each lead, the lower bound is still above the median signal accuracy, meaning even their worst day is better than average. Smith attributes this to the time savings AI scoring provides their night technicians to focus on quality and care, and of course, their outstanding training program.
A third area where SMS excels in their use of technology is in the process of gathering sleep data. In a PSG study, the night tech will monitor a patient’s brain waves, eye movements, heart rate, breathing patterns, blood oxygen level, their limb and body movements, as well as any other movements or noises, such as snoring or sleep walking. As part of this process, night techs must monitor a lot of sensors on a person, as demonstrated in the photo to the right.
For the non-sleep techs in our reading audience, among the data points that are gathered in a PSG, a patient will typically have eight EEG leads on their head. In the above photo, you can see two of these eight leads on the forehead, which would translate to F3 and F4 in the below chart. As you can see below, when it comes to collecting data from these specific leads, the SMS team truly stands out, in a good way. Across all eight of the electrodes, their team consistently collects data at a rate higher than their peers.
As you can see below, for the eight signal leads on the head during a PSG, SMS’s signal accuracy is consistently above the 75th percentile among their peers. Not only that, but for each lead, the lower bound is still above the median signal accuracy, meaning even their worst day is better than average. Smith attributes this to the time savings AI scoring provides their night technicians to focus on quality and care, and of course, their outstanding training program.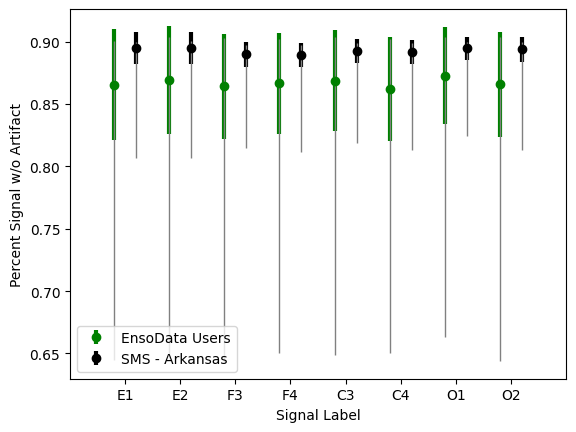
Time for Monitoring, Training Leads to Success
EnsoSleep provided the SMS scoring team with the ability to initiate recording quality initiatives, which helped improve the patient-experience. In the new business model, techs have fewer tasks vying for their attention during the testing process, so they can focus all of their mental energies on monitoring the patient. The result of this dedication? Outstanding data gathering capabilities, as evidenced above. But you can’t simply walk in off the street and perform at peak levels. SMS prides itself on an outstanding training staff that gets night techs the tools they need to be successful. “When new technical staff are hired, they train with the best of the best. Our clinical coordinator, Jurgen Ratliff gets regular feedback and puts a plan in place to address any areas that might need more attention.” said Smith. “I really don’t feel that we lose any quality thanks to our workflow processes.” One of those processes for SMS is leveraging a 3:1 patient:tech ratio. Yes, those outstanding data collection numbers come with a strong ratio to boot. Though Smith did highlight the growing acuity levels in patients leading to more circumstances that require one on one testing. “We know that some patients require more attention. For patients with higher acuity levels, we will schedule 2:1 or even 1:1 appointments based on acuity levels,” said Smith. Higher acuity patients in-lab are another area where the value of time can really improve the patient experience, and SMS focuses on providing that time to each and every sleep patient in their network.Scalable Growth is the End Game
As SMS continues to add labs, Smith has found that the changes SMS has made with technology and processes led to an easier transition for incumbent teams during acquisitions. In retraining staff of acquired organizations, SMS emphasizes the focus on patient care as the priority, rather than on scoring on the fly, as techs might be accustomed to from past experiences with other organizations.AI scoring changed the way our night techs think about their work,” added Smith. “Utilizing EnsoSleep allowed more time for experienced scoring staff to work one on one with night staff to address any recording quality issues.”And as we mentioned above, when patients do require more attention, SMS will schedule a 2:1 or 1:1 ratio appointment. In addition, the clinical team is always on call for the night staff, available to address anything that may come up. Remote monitoring technology allows the team to remote in and review the study in real time with technical staff if needed. And each morning, the day techs have a reliable AI scored study to begin with, one that has impeccably collected data to help clinicians make the right diagnoses.
Parting Advice from Smith, Plus Other Reading:
When asked about the one thing other IDTF operators, private sleep lab owners, and even health system sleep program directors can do to improve their sleep operation, Smith advocated for technological evolution, offering this piece of advice:Embrace technology and change. If you’re standing still, you’re not growing,” Smith recommended.We couldn’t agree more, Susan. Thank you so much for taking the time to share your sleep story and the value of embracing technology for the better. If you’d like to check out another sleep story, here are a few others from the past year:
- Ease of Use Results in Better Patient Care at WellSpan
- Two-thirds of a Lifetime focused on Sleep
- A True Mentor for Sleep Professionals
- The Voice of Sleep Review and Sleep Medicine
- Two Decades Striving for Better Sleep Health






