AI and Sleep Medicine: Where the Market is Headed
Today, we will be discussing AI and sleep medicine, the current relationship between them and how AI might transform sleep medicine going forward. We’re basing this piece off an excellent
Sleep Review webinar hosted last week. Presenters included
Dr. Nate Watson, MD, MSc.,
Dr. Emmanuel Mignot, MD, PhD, and
Dr. Jon Agustsson, PhD.
Each sleep professional spent 15-20 minutes talking through a few slides, and then the trio participated in a Q&A to wrap up the informative webinar. In this post, we will dive into the insights of just one of our esteemed experts, leaving you to
indulge in the full webinar on your own. And, if you want to catch the second part in this series, “
Sleep Medicine and Machine Learning: The AI Revolution,” we examine the insights presented by Dr. Mignot in more detail, (outlined by our Marketing Manager, Steven here below). And if you’d like to check out the
Nox Medical site, you’ll find an overview from Dr. Agustsson.
With that said, let’s dive into the thoughts on the future of AI and sleep medicine, as presented by Dr. Nate Watson.
The Limitations of Human Assessment
In the US, we are collectively performing 25M sleep electroencephalograms (EEGs) and 4M polysomnography tests (PSGs) each year. We visually assess this sleep data using our standardized scoring rules, and we’ve had success in this format for years. However, the human physiological state is incredibly complicated. By some estimates, it contains trillions of information points beyond our comprehension and beyond our genetic code. The beauty of an AI solution is that it can take more data points into account than the human brain can process.
Take the photo example shared by Dr. Watson. This beautiful jungle forest has clear, obvious characteristics that can be easily seen: moss, trees, fog, and ferns. For Dr. Watson, this first view of the picture is akin to a human reviewing an EEG test manually, spotting what we expect to see. However, when giving it a more detailed look, you see hidden images within the picture: an elephant on the right side, a jaguar in the front, middle tree, an orangutan on the right side and a tree sloth on the tree above the jaguar, among others hidden in the photo.

These “under-appreciated” aspects don’t jump off the page immediately, and each human will likely notice different animals and data points first. While the human brain and eyes may not recognize each of these animals immediately (or ever), an AI system will have triggers going off announcing something is different, unique, and worth a more detailed look from the clinician reviewing the data. In the reverse, just as a human easily sees the moss, trees and jungle atmosphere, an AI system might miss these elements. Together, expert sleep technicians and AI can understand the whole picture.
Machine Learning for Automated Scoring & Analysis of PSG Data
The complexity of the problems AI is trying to solve requires inputting a vast number of information points. Take the EEG, for example. The EEG is a current measure of the physiological state of your brain. There’s a lot of talk about machine learning PSG scoring, and one concern that pops up is the accuracy of AI scoring compared to human scoring.
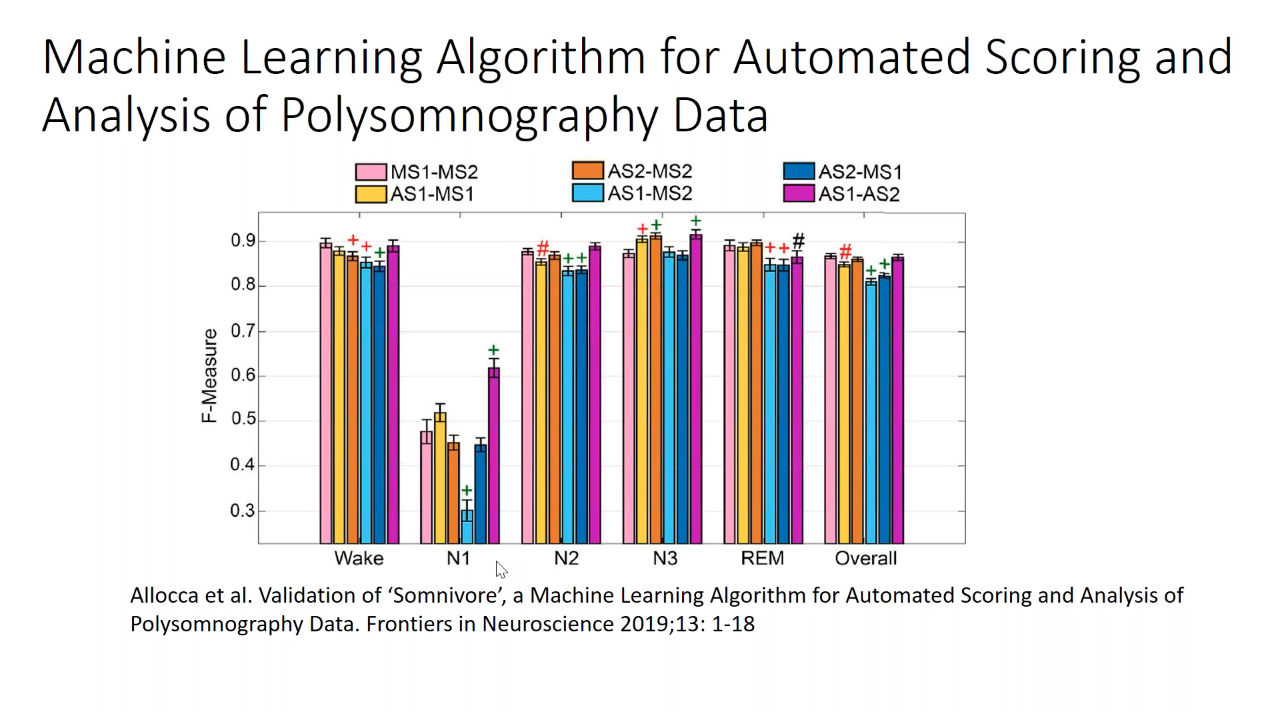
There are a number of studies that demonstrate the accuracy of AI scoring, and Dr. Watson included data in his presentation on a few important studies. In one example, you can observe strong correlations between the human scorers and AI scorers, outlined below. While N1 is a bit of a challenge for all assessors, the remaining and overall categories demonstrate very similar scoring results, with AI systems maintaining similar levels as their human counterparts.

In another study, the researchers go a step further, not only looking at sleep staging, but also apnea detection, AHI categorization, and limb movement detection. Again, the data speaks to the ability of AI to measure and score studies with the same level of accuracy as human counterparts. You can see in the data below, for Sleep Staging, the agreement is 0.85 or greater for all sleep stages, (with the exception of N1). For the apnea detection and limb movement detection, you can see really strong correlations, both holding an r2 above a 0.79. Based on a number of studies, Dr. Watson was confident in the ability of machine learning and AI to score sleep studies, outlining that the improvement of AI accuracy should help ease one major concern for sleep centers and health systems when considering an AI implementation.

What the EEG means for the Future
With all of the insights gained from an AI evaluation of data, there are often opportunities that the human interpreter isn’t considering. This raises the question, “what if we focus on the EEG alone?” He cites two recent studies as he looks at different ways to derive value from EEG data. Each study demonstrates strong promise for the future of AI.
Our own study, “
Using Novel EEG Phenotypes and Artificial Intelligence to Estimate OSA Severity,” looks at how artificial intelligence and machine learning can extract the neurological phenotypes that correlate with sleep disorders by analyzing overnight EEG recordings. With over 4,650 patients in the study, our team looked at EEG sleep studies from a large clinical dataset. Ultimately, the study demonstrated a promising opportunity to estimate OSA severity with a host of EEG study types using applied artificial intelligence. Dr. Watson discusses the insights of this study in more detail starting at the 10:28 mark of the presentation.
In the second study referenced by Dr. Watson, “
Brain Age From the Electroencephalogram of Sleep,” (Sun et al.), the research team sought to assess the ability of AI to predict and analyze brain ages based on EEG data. Per the study abstract, “The human EEG of sleep undergoes profound changes with age. These changes can be conceptualized as “brain age,” (BA), which can be compared to chronological age to reflect the degree of deviation from normal aging.” Per Dr. Watson, brain age serves as a potential aging biomarker, where the variation of BA between people of the same chronological age may be predictive of risks of cognitive decline or psychiatric disease, including Alzheimer’s, schizophrenia, epilepsy, bipolar disorder and others. The machine learning model was trained on 2,532 individuals from Massachusetts General Hospital and 1,974 from the Sleep Heart Health Study.
Like our study, the ability of AI to analyze micro-level data points in the Sun et al. study goes beyond the macro-level data, providing opportunities far beyond human levels currently. For Dr. Watson, this study further demonstrates the real future of a pre-clinical marker for health to help decide when to intervene. “If we have neuroprotective agents, this may allow us to use the EEG to assess brain health over time and to assess the impact of interventions on brain health,” he concludes. You can find Dr. Watson’s full analysis on the Sun et al. study at the 13:45 mark of the presentation.
In both of these studies, the takeaway was clear: AI has the ability to analyze more complex data, and the ability to find correlations between EEG information and other known health disorders of all kinds. The thing that excites both Dr. Watson and our team the most about this is the possibility of phenotypic determination.
What is the limit for AI and Sleep Medicine?
These studies really have Dr. Watson contemplating phenotypic determinism, a fairly new concept that goes deeper into the effects of “nature and nurture” on individuals. To explain it in layman’s terms, we’ll outline a few things. First, your genotype is simply your genetic composition: your genes. Your environment includes all the physical, chemical and biological factors external to you. Combining the two creates a phenotype, or a set of observable traits you might share with others with a similar genotype and environment.
Analyzing phenotype data led to the concept of genetic determinism, a belief that human behavior is controlled by your genes far more than your environment. Per Dr. Watson, we’ve lived in a time of genetic determinism for a while, as we use large datasets to help us better predict human diseases. When you add in the fact that consumers are seeking more personal information daily, leading to the “time of the quantified self,” the opportunity for AI to support clinicians is ripe. Consumers want to be able to measure themselves and understand themselves better, and they’re clamoring for efficient, easy ways to do so.
This perfect storm of consumer interest, clinic need, and technological availability is here to help create true, phenotypic determinism through AI. Per Dr. Watson, once AI gets to the point where it can integrate everything, (genomics, transcriptomics, metabolomics), along with all the various environmental factors that could be out there, elements of the quantified self, and put all this together, the capabilities are potentially limitless.
Improving the Doctor / Patient Relationship
According to Dr. Watson, the impact of AI technology on society and consumers could be massive. From having the necessary healthcare information about jobs and living locations, consumers will have more choice. In an example, Dr. Watson outlines a cost benefit analysis that might include AI insights for patients. Does the proximity of your house to known health situations have a stronger impact on you? Might adverse work conditions be even more dangerous due to a previous condition? Because AI has the ability to identify risk more accurately, consumers will have more information about their own phenotype and will be able to make better life choices.
From a medical perspective, Dr. Watson believes AI will take doctors back to the future. There are distractions in the doctor / patient relationship that can be changed for the better thanks to AI. Doctors can be more engaged with patients, as AI manages certain aspects of a visit. Dr. Watson also highlights the recent position statement from the
American Academy of Sleep Medicine.
“While AI applications are expected to improve sleep lab efficiency and yield greater clinical insights, the goal of AI integration is
to augment, not replace expert evaluation of sleep data,” paraphrased Dr. Watson. “The big plus [of AI] is the notion of sub-phenotyping patients. We must not view sleep apnea as just one monolithic disease, but we understand that each patient is unique, and we’re able to address that uniqueness in order to tailor therapies to maximize efficacies of treatment and positive outcomes.”
AI scoring currently is still only being deployed as an augmented source, with skilled technician’s monitoring the sleep technology. However, the future of AI will be determined by those who chose to use it and invest in it from the get go.
Ultimately, what does AI mean for Sleep Medicine?
To close, we go back to Dr. Watson for another pop-culture example, this time from the Matrix. He mentions the red pill v. blue pill decision the protagonist Neo must make. In the blockbuster, Neo can choose to take a red pill, and embrace the future, or choose to take the blue pill, and remain blissfully unaware of what is happening in the world around him.

“I think AI is presenting this question to the sleep community. We know that we don’t have enough board certified sleep doctors to take care of all sleep disease that’s out there in the world. We know 70 million people in the U.S. alone have a sleep issue, and 60% of them have a sleep disorder,” said Dr. Nate Watson. “We know there’s one board certified sleep doctor for every 45,000 citizens, so there’s no doubt that we need to increase access to diagnostic modalities in treatment for individuals that right now aren’t getting taken care of. So, I’m going to suggest we swallow the red pill, and move forward from here to see what this technology can do for us.”
We couldn’t agree more. To contact our team to talk about how an AI solution can help simplify the lives of your team or allow you to scale your sleep business,
send us a message. We want to be your co-pilot, because a good AI sleep scoring technology in the hands of an awesome sleep staff is an avenue for growth in the short and long term.
If you enjoyed the post, we encourage you to
share it on Twitter or on your favorite social channel, tagging @EnsoData.
For those of you who have made it this far, you might be interested in our other recent blog content:
 These “under-appreciated” aspects don’t jump off the page immediately, and each human will likely notice different animals and data points first. While the human brain and eyes may not recognize each of these animals immediately (or ever), an AI system will have triggers going off announcing something is different, unique, and worth a more detailed look from the clinician reviewing the data. In the reverse, just as a human easily sees the moss, trees and jungle atmosphere, an AI system might miss these elements. Together, expert sleep technicians and AI can understand the whole picture.
These “under-appreciated” aspects don’t jump off the page immediately, and each human will likely notice different animals and data points first. While the human brain and eyes may not recognize each of these animals immediately (or ever), an AI system will have triggers going off announcing something is different, unique, and worth a more detailed look from the clinician reviewing the data. In the reverse, just as a human easily sees the moss, trees and jungle atmosphere, an AI system might miss these elements. Together, expert sleep technicians and AI can understand the whole picture.
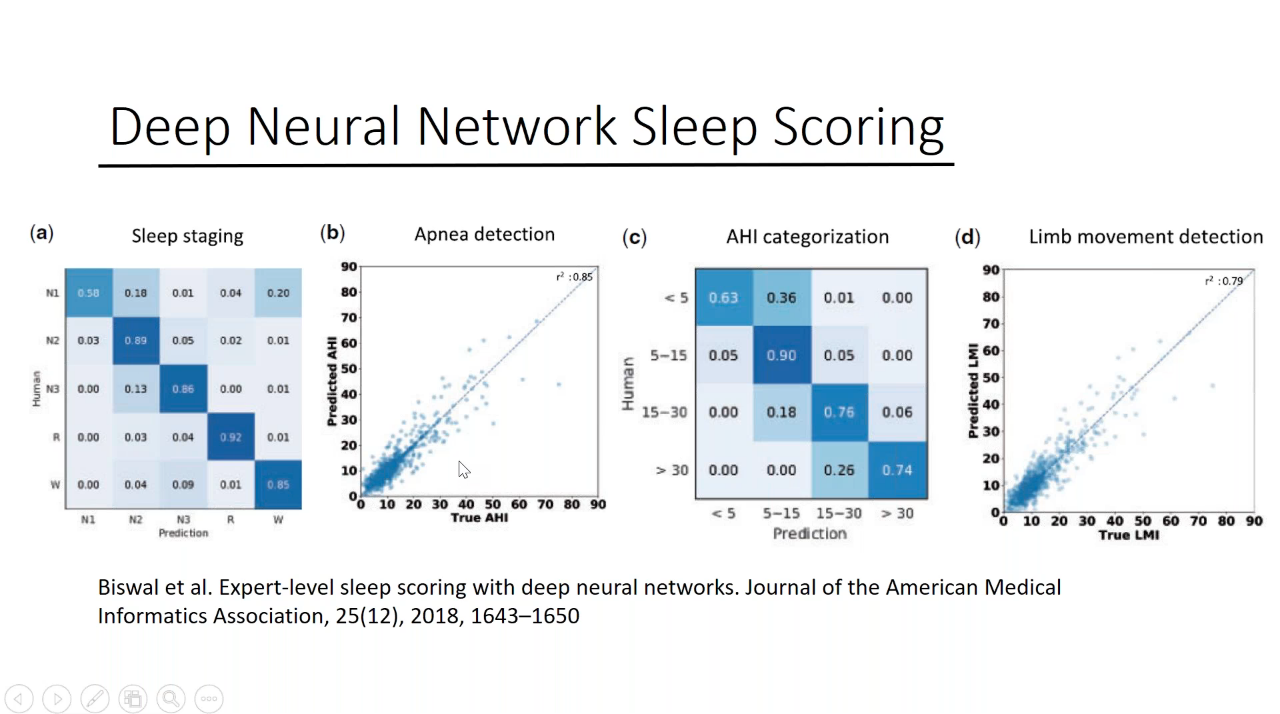
 In another study, the researchers go a step further, not only looking at sleep staging, but also apnea detection, AHI categorization, and limb movement detection. Again, the data speaks to the ability of AI to measure and score studies with the same level of accuracy as human counterparts. You can see in the data below, for Sleep Staging, the agreement is 0.85 or greater for all sleep stages, (with the exception of N1). For the apnea detection and limb movement detection, you can see really strong correlations, both holding an r2 above a 0.79. Based on a number of studies, Dr. Watson was confident in the ability of machine learning and AI to score sleep studies, outlining that the improvement of AI accuracy should help ease one major concern for sleep centers and health systems when considering an AI implementation.
In another study, the researchers go a step further, not only looking at sleep staging, but also apnea detection, AHI categorization, and limb movement detection. Again, the data speaks to the ability of AI to measure and score studies with the same level of accuracy as human counterparts. You can see in the data below, for Sleep Staging, the agreement is 0.85 or greater for all sleep stages, (with the exception of N1). For the apnea detection and limb movement detection, you can see really strong correlations, both holding an r2 above a 0.79. Based on a number of studies, Dr. Watson was confident in the ability of machine learning and AI to score sleep studies, outlining that the improvement of AI accuracy should help ease one major concern for sleep centers and health systems when considering an AI implementation.
 “I think AI is presenting this question to the sleep community. We know that we don’t have enough board certified sleep doctors to take care of all sleep disease that’s out there in the world. We know 70 million people in the U.S. alone have a sleep issue, and 60% of them have a sleep disorder,” said Dr. Nate Watson. “We know there’s one board certified sleep doctor for every 45,000 citizens, so there’s no doubt that we need to increase access to diagnostic modalities in treatment for individuals that right now aren’t getting taken care of. So, I’m going to suggest we swallow the red pill, and move forward from here to see what this technology can do for us.”
We couldn’t agree more. To contact our team to talk about how an AI solution can help simplify the lives of your team or allow you to scale your sleep business, send us a message. We want to be your co-pilot, because a good AI sleep scoring technology in the hands of an awesome sleep staff is an avenue for growth in the short and long term.
If you enjoyed the post, we encourage you to share it on Twitter or on your favorite social channel, tagging @EnsoData.
For those of you who have made it this far, you might be interested in our other recent blog content:
“I think AI is presenting this question to the sleep community. We know that we don’t have enough board certified sleep doctors to take care of all sleep disease that’s out there in the world. We know 70 million people in the U.S. alone have a sleep issue, and 60% of them have a sleep disorder,” said Dr. Nate Watson. “We know there’s one board certified sleep doctor for every 45,000 citizens, so there’s no doubt that we need to increase access to diagnostic modalities in treatment for individuals that right now aren’t getting taken care of. So, I’m going to suggest we swallow the red pill, and move forward from here to see what this technology can do for us.”
We couldn’t agree more. To contact our team to talk about how an AI solution can help simplify the lives of your team or allow you to scale your sleep business, send us a message. We want to be your co-pilot, because a good AI sleep scoring technology in the hands of an awesome sleep staff is an avenue for growth in the short and long term.
If you enjoyed the post, we encourage you to share it on Twitter or on your favorite social channel, tagging @EnsoData.
For those of you who have made it this far, you might be interested in our other recent blog content:






